Rajkumari, a 17-year-old from Pokhari Village, in Uttarakhand, India, grew up believing that she had inherited an evil spirit. She was haunted by stories of her uncle, who suffered from the same unexplained convulsions and passed away before she was born. Treatment for her condition was in the hands of a local traditional doctor because medical care in her remote area was almost impossible to access, much less afford. To avoid the stigma associated with her convulsions, Rajkumari retreated into the home she shared with her mother.
She later learned that her inherited "spirit" was epilepsy, a treatable neurological condition that affects nearly 50 million people globally, about 80% of whom reside in low- or middle-income countries (LMICs). What Rajkumari didn't realize was that her seizures were part of a neglected global health crisis that almost claimed her life. This hidden danger manifested tragically one day as she was cooking over an open fire.
The flickering flame triggered a seizure: Proximity to the light patterns of fire are a common cause of an epileptic episode. This caused her to fall unconscious into the blaze, remaining in the fire, until her mother returned home and found her. She sustained severe burns across her face, lost sight in her right eye, and suffered extensive skin damage.
This horrific scenario is tragically common yet underreported. Burn injuries are the leading cause of morbidity and mortality among epileptic patients, particularly in LMICs, where 40% of the world's population still rely on open fires for cooking, for heat, and even as a light source. Women and children, in particular, are at high risk for burn injuries because of more time spent at home and cooking.
Rajkumari didn't know that her condition could be triggered by an open flame—and she's not alone. One study found that the greatest risk factors for the increased incidence of burns in epileptic patients were not just the frequency or duration of seizures, but also the general lack of awareness and education about the risk of burns among epileptic patients.
Epilepsy in Context: Gender, Tradition, Stigma, and Access Challenges
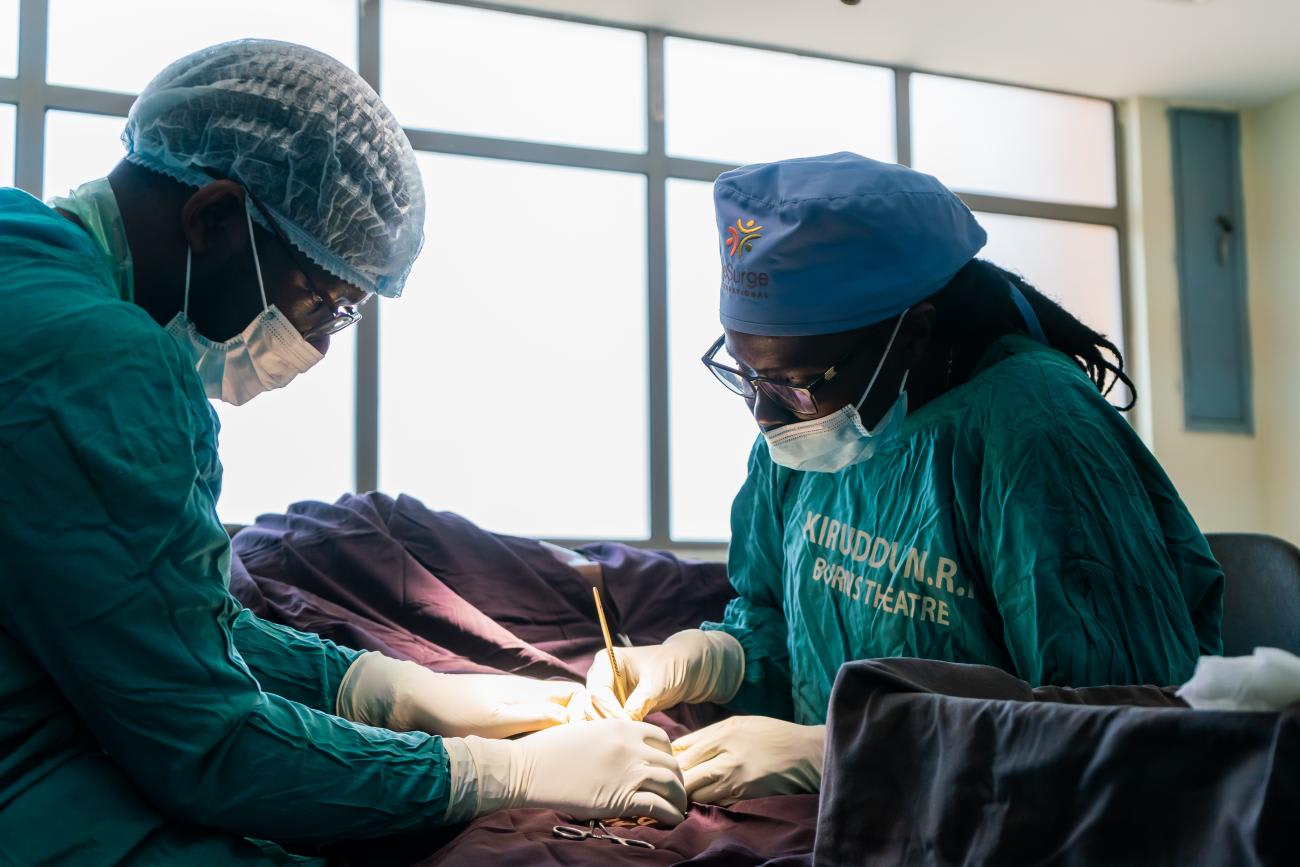
Nearly 4,000 miles away in Uganda, Rose Alenyo observes a similar phenomenon. A plastic and reconstructive surgeon collaborating with ReSurge International, Alenyo operates out of the country's only burn center at Kiruddu National Referral Hospital, in Kampala, which serves the entire population of 50 million. This facility is crucial given the high prevalence of injuries related to open cooking fires combined with crowded living conditions.
"We treat an average of 92 epilepsy patients in the burn ward yearly, constituting about 18% of our overall burn patient load," Alenyo reports.
Burn injuries are the leading cause of morbidity and mortality among epileptic patients, particularly in LMICs
Gender plays an outsized role in increasing the risk of burns for women with epilepsy. The majority of Alenyo's patients are women ages 15 to 25 who live in single-room dwellings within urban slums and often cook at home with open flames.
"Epilepsy is so stigmatized that the women or their families won't disclose it," says Alenyo, adding that young girls are expected to cook. "When cooking, she can be triggered and will be burning unconscious until someone comes by," just like Rajkumari and her mother. "By the time they come to our center, it is usually the fifth burn, and they've finally come because it is so severe," says Alenyo.
Beyond the immediate physical injuries caused by burns, these women also face the ongoing mental toll of managing or hiding frequent seizures. Burn injuries from the seizures can also add new disabilities and disfigurement, often increasing their dependence on others for daily survival. The mental and emotional toll of dealing with severe burn scars can add an extra layer of stigmatization and obstacles for participating in society. That reliance exacerbates social and economic burdens on families and communities.
"We are confronted daily with their heartbreaking stories, their lost dreams, and the profound stigma they face," she says, underscoring that many of these incidents are largely preventable. The stigma, especially for women, is a critical factor preventing epilepsy patients from accessing care. The World Health Organization estimates that up to 70% of people living with epilepsy could live seizure free given proper diagnosis and treatment. However, the condition often goes unrecognized as a medical issue because a combination of medical access and pervasive cultural beliefs and superstitions strongly influence perceptions and treatments of epilepsy across LMICs.
"Most of our epileptic burns are from villages where epilepsy is believed to be caused by witchcraft or evil spirits and [is] treated by spiritualists or traditional healers," explains Alenyo, discussing her cases in Uganda. This story applies globally. In Zimbabwe, epilepsy is often attributed to arohwa nezvinhu—meaning witchcraft used to send bad spirits to attack someone. In India and Nepal, doctors frequently confront superstitions related to bad karma, astrology, and possession, similar to Rajkumari's experience.
Managing epilepsy presents numerous challenges, exacerbated by a combination of stigma, traditional beliefs, access to health care, and the burdensome costs of long-term treatment, all of which are worse in an LMIC setting. Treatment and management of the disease require lifelong medication and regular follow-up care, which makes compliance a major issue. Even if a patient can adhere to long-term medications, they may have to travel long distances—sometimes two to three hours on foot—just to obtain their prescriptions. Many fear the side effects or are unable to afford lifelong treatments.
In Kenya, for example, the cost of generic medications for epilepsy ranges from $12 to $240 per year for the highest doses. In a country where 36% of the population lives on $2.15 per day or $785 per year, this treatment could cost a household approximately 30% of their income. In India, the annual cost for anti-epileptic medication ranges from $500 to $700 for a single medication and $1,200 to $1,500 for multiple medications. This is an even more exorbitant cost given that 12% of the population lives on $785 annually. Other expenses involve transportation, medical consultations, and in some cases polypharmacy (multiple drugs).
For families already struggling financially, these costs can be overwhelming. As a result, many patients skip doses or stop taking their medication entirely. Without consistent treatment, however, seizure control becomes erratic, increasing the risk of injury and burns.
Awareness, Education, and Access: Solutions to a Complex Problem
Addressing the complex intersection of epilepsy management and burn injuries in LMICs requires a multifaceted approach that goes beyond simply providing care. Awareness, education, and prevention efforts are also necessary. Public health awareness campaigns should focus not only on informing the public about epilepsy and seizure management but also on highlighting the triggers of seizures, including fire.
Education on burn risks, along with other dangers associated with activities, such as operating heavy machinery, should also be prioritized for epileptic patients. First-aid training for burns that target households and caregivers of individuals with epilepsy could greatly reduce the risk of permanent disability or death following an accident. Families and caregivers also need comprehensive education on epilepsy management and the associated risks to support their loved ones.
Systemic health-care challenges, including inadequate access to specialized facilities, inadequate follow-up care, and a lack of educational resources about effective medication management complicate efforts to treat epilepsy. Here, governments have a critical role in enhancing systems and subsidizing medications. Given the barriers to accessing health care, if a patient makes it into the system, they should not be thwarted by the cost of medications.
As health systems work toward implementing those multifaceted, systematic solutions, young women like Rajkumari will continue to suffer
Although ensuring that anti-epileptic medications are available is crucial, patients and their families also need comprehensive education on the need for consistency in taking medication, its role in controlling seizures, and the dangers of noncompliance. Health-care workers can deliver this information during regular follow-up visits, which can take place in mobile health units or via telemedicine in areas where access to health care is limited.
Expanding access to health care and education can be achieved through better patient care coordination, assisted by data management systems to track patients and their treatment plans, ensuring that those at high risk are given the support and restrictions necessary to protect their health and safety.
Examples of complex noncommunicable diseases being integrated into health systems can be seen in programs such as AMPATH in Western Kenya that uses electronic medical records for an integrated health information system. HIV/AIDS programs similarly encounter challenges tracking patients needing long-term, complex care. Malawi's Integrated Chronic Care Clinic, which uses scheduled screenings and referrals for detection and management, also provides a hopeful example of success.
Given the superstitions surrounding epilepsy and the current lack of accessibility and affordability, traditional healers are often the first line of care, thus playing a critical role in their community health provisions. Despite this, their care often exacerbates health outcomes, given that traditional treatments may lack the efficacy of scientifically tested therapies and sometimes contradict medical advice. Traditional healers may also inadvertently perpetuate stigma or harmful practices related to certain diseases, including epilepsy, which can deepen social isolation for patients. Integrating traditional healers within formal health-care systems through collaboration and education may be a path toward improving health outcomes while respecting cultural practices.
As health systems work toward implementing those multifaceted, systematic solutions, young women like Rajkumari will continue to suffer.
Even though her untreated epilepsy resulted in a horrific burn accident, Rajkumari was fortunate to have access to free and readily available health care provided by local surgeon Kush Aeron and financially backed by nongovernmental organizations including ReSurge International and Helping Hands. Rajkumari's path to recovery has been long—her initial injury required five months of intensive care. As her scars form and her healing continues, both physically and emotionally, she will need at least five more reconstructive surgeries for her nose, eyelids, and a corneal transplant.
Today Rajkumari stands tall. In her recovery, she has found joy in caring for her kitten, Whisky, a gift from her uncle and sister, her caretakers. She also reignited her passion for cooking, mastering dishes such as dal, chapatis, and rice without fear of open flames. She says with confidence, "I know now that my seizures were not caused by spirits, and I have support."
As Rajkumari continues to heal, she embodies the spirit of a princess—the meaning of her name in Hindi—crowned by her courage and resilience. Her story serves as a call to action, highlighting the urgent need for global efforts to prevent unnecessary epilepsy-related burn injuries and ensure access to dignified care for all.

AUTHORS' NOTE: Rajkumari's story is part of ReSurge International's Closing the Gap campaign that showcases people whose lives were transformed through reconstructive surgery.












